Sleep is one of the most critical recovery processes your body goes through each night — and the amount of oxygen in your blood while you’re asleep plays a bigger role in that recovery than most people realize. If you’ve been waking up tired, experiencing morning headaches, or recently had a sleep evaluation, you may be wondering: what is normal blood oxygen level during sleep, and is mine where it should be?
The good news is that understanding your blood oxygen level while sleeping doesn’t require a medical degree. With a little clarity on how oxygen saturation works during different sleep stages, what the healthy ranges look like, and when levels become a concern, you’ll be much better equipped to have informed conversations with your healthcare provider.
In this guide, we cover normal oxygen levels during sleep, what causes overnight dips in saturation, and what steps you can take if your levels are outside the ideal range.
What Is Normal Blood Oxygen Level While Sleeping?
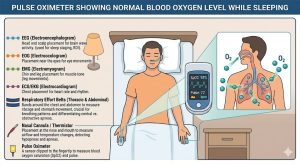
Blood oxygen saturation — measured as SpO₂ — refers to the percentage of hemoglobin in your red blood cells that is carrying oxygen. Think of it as how “full” your blood’s oxygen carriers are. A pulse oximeter, the small clip-on device often placed on a fingertip, can measure this non-invasively.
For most healthy adults, what is normal blood oxygen level while awake is 95–100%. During sleep, it’s normal for this number to dip slightly due to slower, more shallow breathing — but healthy individuals generally maintain saturation levels at or above 95% throughout the night.
Normal Oxygen Level While Sleeping by Age and Health Status
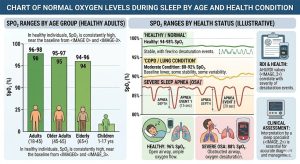
While 95–100% is the widely accepted benchmark, context matters:
- Healthy adults and children: SpO₂ of 95% or higher is considered normal
- Older adults: Some physicians allow for readings as low as 94% without immediate concern, particularly in patients with no underlying respiratory conditions
- Individuals with chronic lung conditions (e.g., COPD): Baseline targets may be adjusted by a physician, often 88–92%
- During REM sleep: Brief, minor dips below 95% can occur even in healthy individuals and are generally not clinically significant
What’s more important than any single reading is the pattern. Sustained drops or frequent fluctuations in overnight oxygen saturation are what prompt clinical concern.
How Does Oxygen Level While Sleeping Change Throughout the Night?
Your oxygen level while sleeping isn’t static — it naturally shifts as you cycle through different sleep stages. Understanding this helps put individual readings in context.
Sleep Stages and Oxygen Saturation
- NREM (Non-REM) sleep: Breathing is slow and regular during these stages. Oxygen saturation typically remains stable and near waking levels.
- REM sleep: This is the stage associated with dreaming. Breathing becomes more irregular, and SpO₂ may dip slightly — typically no lower than 95% in healthy individuals.
- Sleep onset: As the body transitions from wakefulness to sleep, some brief fluctuations in breathing and oxygen levels are normal.
For most people, these natural variations are nothing to worry about. However, if you have an underlying condition such as obstructive sleep apnea, central sleep apnea, or chronic obstructive pulmonary disease (COPD), your oxygen saturation may drop more significantly and more frequently during the night — a phenomenon called nocturnal hypoxemia.
A closely related metric, the oxygen desaturation index, tracks how often per hour your SpO₂ drops by 3–4% or more during sleep. This index is often used alongside blood oxygen data to paint a more complete picture of nighttime respiratory health.
What Is a Dangerously Low Oxygen Level While Sleeping?
This is one of the most important questions to understand. While small, brief dips in overnight oxygen saturation are normal, sustained or severe drops are a different matter entirely.
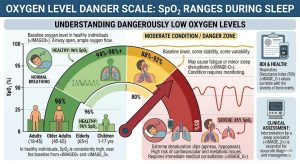
Here’s a practical breakdown of oxygen saturation thresholds:
- 95–100%: Normal range. No intervention typically needed.
- 91–94%: Mildly below normal. May warrant monitoring or further evaluation, especially if symptoms are present.
- 86–90%: Moderate hypoxemia. Clinically significant and should be discussed with a physician.
- 85% or below: Considered severe hypoxemia. This is the threshold most clinicians consider critically low and requiring prompt medical attention.
When it comes to what is a dangerously low oxygen level while sleeping, repeated drops below 90% — even if brief — are generally considered medically significant. Prolonged exposure to SpO₂ levels below 88% can put strain on the heart, impair cognitive function over time, and disrupt the restorative processes that sleep is supposed to provide.
Common warning signs that your oxygen levels may be dipping too low at night include: waking frequently, loud snoring, gasping or choking sounds during sleep (reported by a bed partner), morning headaches, persistent daytime fatigue, and difficulty concentrating.
What Causes Low Oxygen Levels During Sleep?
Several conditions and factors can contribute to reduced oxygen level while sleeping:
- Obstructive sleep apnea (OSA): The most common cause. The airway repeatedly collapses, causing breathing to pause and oxygen to drop.
- Central sleep apnea: The brain fails to send proper signals to the breathing muscles, leading to pauses in respiration.
- Chronic obstructive pulmonary disease (COPD): Reduces the lungs’ ability to efficiently transfer oxygen into the bloodstream.
- Asthma: Can cause airway constriction that limits oxygen intake, particularly during nighttime.
- Heart failure: Affects how efficiently oxygenated blood is circulated throughout the body.
- Obesity: Excess weight can restrict chest expansion and diaphragm movement during sleep.
- High altitude: Ambient oxygen levels are lower at elevation, which can reduce SpO₂ even in healthy individuals.
If you suspect any of these conditions may be affecting your overnight saturation, the first step is a proper sleep evaluation. An at-home sleep test is a convenient, non-invasive way to gather meaningful data about your breathing and oxygen levels while you sleep — without an overnight clinic visit.
What to Do If Your Overnight Oxygen Levels Are Low
If your sleep study results or home monitoring data show that your oxygen saturation is consistently dipping below normal, here’s a general framework for next steps:
Step 1: Talk to a Sleep Specialist
A physician or board-certified sleep specialist can review your oxygen saturation data alongside other metrics — such as your apnea-hypopnea index or respiratory disturbance index — to determine whether a formal diagnosis applies and what treatment is most appropriate.
Step 2: Consider PAP Therapy
Continuous positive airway pressure (CPAP) is one of the most effective treatments for obstructive sleep apnea and nocturnal hypoxemia. If you’ve already been diagnosed and need to update your treatment plan, a CPAP prescription renewal may be a convenient next step.
Step 3: Address Underlying Conditions
Treating the root cause — whether that’s weight management, asthma control, or heart health — often has a meaningful impact on nighttime oxygen levels. Work with your primary care provider to develop a comprehensive plan.
Step 4: Start With a Home Sleep Test
Not sure where you stand? An at-home sleep test can provide clinically meaningful data about your oxygen saturation patterns during sleep. It’s an accessible, affordable first step toward understanding your nighttime health.
Conclusion: Know Your Numbers, Protect Your Sleep
Your blood oxygen level while sleeping is a vital indicator of how well your body is recovering each night. For most adults, a healthy SpO₂ sits between 95% and 100%, with brief, minor dips being a normal part of the sleep cycle. However, sustained drops — especially below 90% — can signal an underlying condition that deserves attention.
Understanding normal oxygen levels during sleep is the first step. The next is knowing where your levels actually stand. Whether you’re experiencing symptoms like daytime fatigue, morning headaches, or disrupted sleep, or you simply want peace of mind, an at-home sleep test gives you a clinically meaningful baseline — conveniently, from your own bedroom. Take control of your sleep health today.
Frequently Asked Questions
What SpO₂ level is too low during sleep?
Most clinicians consider SpO₂ levels consistently below 90% during sleep to be clinically significant. Levels at or below 85% are generally regarded as severely low and warrant prompt medical evaluation.
Can a pulse oximeter be used to monitor oxygen while sleeping?
Yes. Consumer-grade pulse oximeters can provide a helpful snapshot of your overnight oxygen saturation. However, for a clinically validated assessment — especially one that accounts for breathing events, snoring, and sleep stages — a formal sleep study or home sleep test is more comprehensive and reliable.
Does sleeping position affect blood oxygen levels?
It can. Sleeping on your back (supine position) may worsen airway obstruction in individuals with sleep apnea, leading to more frequent oxygen dips. Many patients find that sleeping on their side (lateral position) helps maintain more stable oxygen saturation throughout the night.
Can low oxygen levels during sleep cause long-term health problems?
Yes, if left untreated, chronic nocturnal hypoxemia is associated with elevated cardiovascular risk, increased blood pressure, impaired cognitive performance, mood disturbances, and reduced quality of life. Early detection and treatment are key to preventing these outcomes.
Is 94% a normal oxygen level while sleeping?
For most healthy adults, 94% is slightly below the ideal range of 95–100%. A single reading at 94% may not be concerning, but if you’re consistently measuring at this level or below throughout the night, it’s worth discussing with your physician, particularly if you have any underlying health conditions or sleep-related symptoms.